
4. ADA, EASD consensus report 2019
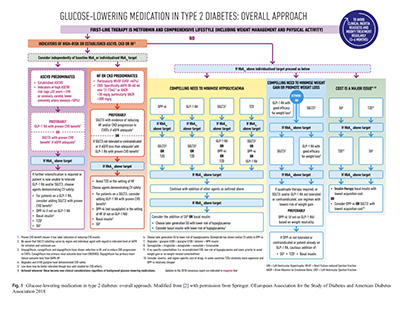
A consensus report by the American Diabetes Association (ADA) and the European Association for the Study
of Diabetes (EASD) on the Management of hyperglycaemia in type 2 diabetes.
The ADA and the EASD have briefly updated their 2018 recommendations on management of hyperglycaemia,
based on significant research findings from large cardiovascular outcomes trials published in 2019.
Important changes include suggestions that treating high-risk individuals with a glucagon-like-peptide
1 (GLP-1) receptor agonist or sodium–glucose cotransporter 2 (SGLT2) inhibitor to reduce major adverse
cardiovascular events (MACE), hospitalisation for heart failure (hHF), cardiovascular death or chronic
kidney disease (CKD) progression should be considered independently of baseline HbA1c or individualised
HbA1c target.
The consensus suggests that GLP-1 receptor agonists can be considered in patients with type 2 diabetes without established CVD with indicators of high risk, specifically, patients aged 55 years or older with coronary, carotid or lower extremity artery stenosis >50%, left ventricular hypertrophy, an eGFR.
SGLT2 inhibitors are recommended in patients with type 2 diabetes and heart failure, particularly those with heart failure with reduced ejection fraction, to reduce hHF, MACE and CVD death, as well as in patients with type 2 diabetes with CKD (eGFR 30 to ≤60 ml min−1 [1.73 m]−2 or urinary albumin-to-creatinine ratio >30 mg/g, particularly >300 mg/g) to prevent the progression of CKD, h HF, MACE and cardiovascular death. Analysis of two SGLT2 inhibitor CVOTs, DECLARE– TIMI 58 and the Canagliflozin Cardiovascular Assessment Study (CANVAS) Program suggests that the benefits of SGLT2 inhibitors for hHF, MACE and cardiovascular death are greatest for those individuals with preexisting heart failure with reduced ejection fraction (HFrEF) compared with those without HFrEF. The new recommendations also suggest that SGLT2 inhibitors are recommended in patients with type 2 diabetes and HF, particularly those with HFrEF, to reduce hHF, MACE and CV death.
For enquiries info@jothydev.net.
Please visit: jothydev.net | research.jothydev.com | diabscreenkerala.net | jothydev.com/newsletter
